Lithium Toxicity Risk Calculator
How Medications Affect Your Lithium Levels
Lithium has a narrow therapeutic window. Even small increases from common medications can push you into toxic levels. Enter your current lithium level and select which medication you're taking to see potential risks.
Imagine taking lithium every day to keep your mood stable - and then, without realizing it, a simple over-the-counter painkiller pushes your lithium levels into the danger zone. This isn’t a hypothetical scenario. It happens more often than you think. Lithium is one of the most effective treatments for bipolar disorder, but its narrow window between helping and harming makes it one of the most dangerous drugs if not managed carefully. And two of the most common medications people take - diuretics and NSAIDs - can turn a safe dose into a life-threatening one.
Why Lithium Is So Sensitive
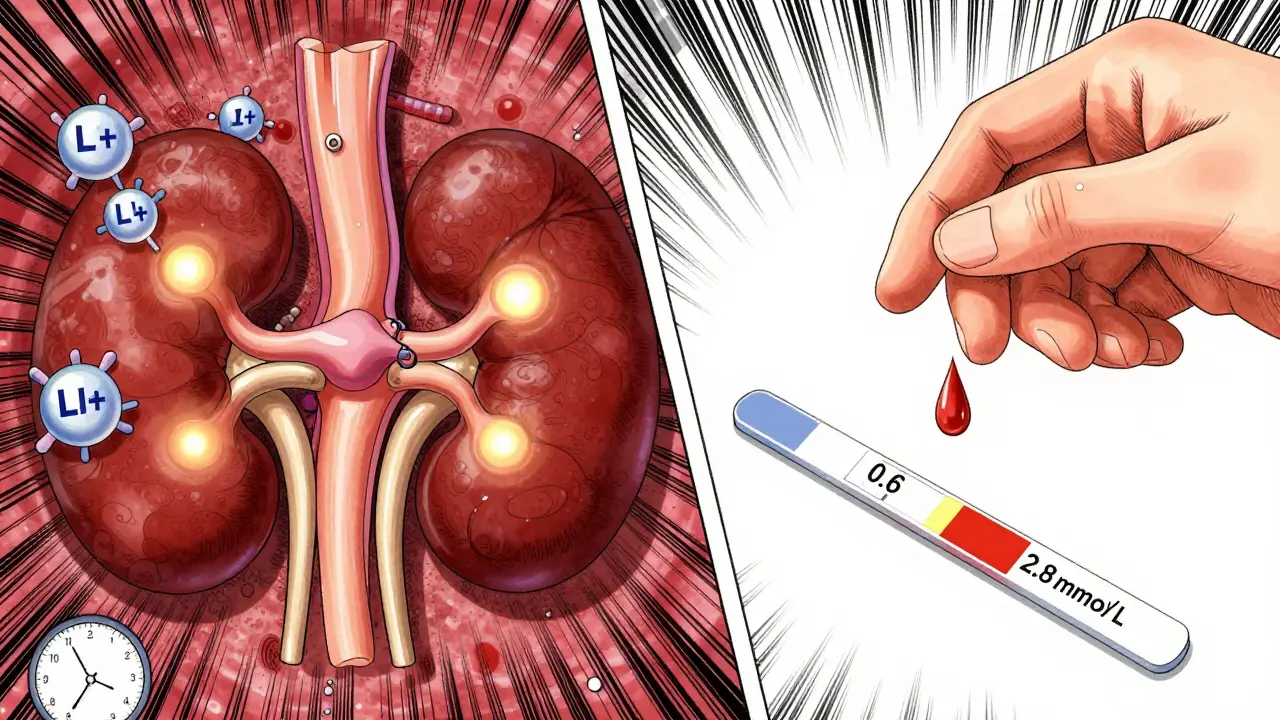
Lithium doesn’t get broken down by your liver. Instead, it passes through your kidneys almost unchanged. That’s why it’s so effective - but also why it’s so risky. Your kidneys filter lithium out of your blood, but they also reabsorb a big chunk of it back into your system. The balance is delicate. Too much reabsorption? Lithium builds up. Too little? It doesn’t work. The safe range is tiny: 0.6 to 1.2 mmol/L. Go above 1.5 mmol/L, and you’re in toxicity territory. At 2.0 mmol/L or higher, you’re at risk of seizures, kidney damage, or even death.
What makes this even more dangerous is that lithium levels can rise without any obvious symptoms at first. You might just feel a little more tired, get a mild tremor in your hands, or have nausea. These are easy to ignore - until they spiral into confusion, slurred speech, or loss of coordination. And by then, it’s often too late.
Diuretics: The Silent Lithium Boosters
Diuretics - water pills - are commonly prescribed for high blood pressure, heart failure, or swelling. But not all diuretics are equal when it comes to lithium. Thiazide diuretics like hydrochlorothiazide and bendroflumethiazide are the worst offenders. They work in a part of the kidney that also handles lithium reabsorption. When they block sodium reabsorption, lithium gets pulled along for the ride. Studies show that thiazides can raise lithium levels by 25% to 40%, sometimes even fourfold.
Here’s the scary part: this doesn’t take weeks. The spike can happen within just 3 to 5 days of starting the diuretic. A 72-year-old woman in New Zealand died after adding a thiazide diuretic to her lithium regimen. Her lithium level jumped from 0.8 mmol/L (safe) to 1.9 mmol/L (toxic) in under a week. She wasn’t monitored closely. That’s the pattern: people start a new medication, assume it’s harmless, and never get their lithium checked again.
Loop diuretics like furosemide are a bit safer. They act higher up in the kidney, so they don’t interfere with lithium reabsorption as much. They still raise lithium levels - usually by 10% to 25% - but the risk is lower, especially if kidney function is normal. For patients who absolutely need a diuretic, furosemide is the preferred choice over thiazides. But even then, monitoring is non-negotiable.
NSAIDs: The Hidden Danger in Your Medicine Cabinet
NSAIDs - nonsteroidal anti-inflammatory drugs - are everywhere. Ibuprofen, naproxen, aspirin. You can buy them without a prescription. And that’s the problem. People take them for headaches, arthritis, or menstrual cramps. They don’t think about lithium. But NSAIDs shut down prostaglandins in the kidney. Prostaglandins help keep blood flow steady to the filtering units. When they’re blocked, kidney filtration drops by 10% to 20%. Lithium, which depends on that flow, gets stuck.
The effect isn’t the same for every NSAID. Indomethacin is the worst - it can push lithium levels up by 20% to 40%. Piroxicam and naproxen aren’t far behind. Ibuprofen? It’s still risky. A typical dose of 600 mg three times a day can raise lithium by 15% to 30%. And in one documented case, a patient’s lithium level hit 2.8 mmol/L after starting ibuprofen. That’s severe toxicity. He needed dialysis because lithium had soaked into his brain and nerve cells - and even after blood levels dropped, the lithium inside his tissues kept leaking out.
Here’s the catch: you don’t need to be on high doses. Even a few tablets of Advil or Aleve over a few days can do it. And if you have reduced kidney function - common in older adults or people with diabetes - the risk jumps even higher. The American Psychiatric Association says: avoid NSAIDs if you can. If you must take them, check your lithium level every 4 to 5 days.
Other Medications That Play a Role
It’s not just diuretics and NSAIDs. ACE inhibitors like lisinopril and ARBs like valsartan - common blood pressure drugs - can raise lithium levels by 15% to 25%. Calcium channel blockers like verapamil don’t change lithium levels much, but they can make neurological side effects like tremors and ringing in the ears much worse. Antidepressants like fluoxetine and sertraline also interact, though the mechanism is less clear.
And what about herbal supplements? The NHS warns: we don’t know. No one has studied whether St. John’s wort, ginkgo, or garlic affect lithium. That uncertainty means the safest rule is this: tell your doctor every single thing you’re taking - pills, powders, teas, or drops.
What to Do If You’re on Lithium
If you’re taking lithium, here’s what you need to do - right now:
- Get your lithium level checked before starting any new medication - even if it’s OTC.
- Never start NSAIDs or diuretics without talking to your psychiatrist or pharmacist.
- Monitor symptoms: tremors, nausea, confusion, frequent urination, or dizziness? Call your doctor. Don’t wait.
- Ask about alternatives: For pain, acetaminophen (Tylenol) is usually safer. For high blood pressure, some medications like amlodipine have less interaction risk.
- Know your baseline: Your kidney function (eGFR) and lithium target level should be written down and reviewed every 3 to 6 months - and every 4 to 5 days after any new drug.
Some patients need diuretics. Some need pain relief. But you can’t just guess. Lithium toxicity doesn’t come with warning signs you can ignore. It creeps up silently. One study found that 65% of psychiatrists use electronic alerts to flag drug interactions - but only 45% actually follow up with the required blood tests. That gap kills.

The Future: Better Monitoring, Safer Lithium
There’s hope. In 2023, the FDA approved a home-testing device called LithoLink™ - a smartphone-connected tool that lets patients check their lithium levels without going to the lab. Results go straight to their doctor. This could change everything for people who live far from clinics or forget appointments.
Researchers are also testing a new form of lithium - nano-encapsulated lithium citrate - that doesn’t rely as heavily on kidney filtration. Early trials show it stays more stable when taken with NSAIDs. That’s huge. If it works, it could make lithium safer for millions.
For now, though, the rules haven’t changed. Lithium saves lives. But it demands respect. You can’t treat it like any other pill. Every new medication - no matter how small or common - is a potential trigger. Your life depends on knowing that.
Can I take ibuprofen while on lithium?
Taking ibuprofen while on lithium is risky. Even a standard dose of 600 mg three times daily can raise lithium levels by 15% to 30%. In some cases, this pushes levels into the toxic range (above 1.5 mmol/L). If you must take ibuprofen, check your lithium level within 4 to 5 days of starting it. Never take it without your doctor’s approval. Acetaminophen (Tylenol) is a safer option for pain relief.
Why are thiazide diuretics more dangerous than loop diuretics with lithium?
Thiazide diuretics like hydrochlorothiazide act on the distal tubule of the kidney - the same area where lithium is reabsorbed. By blocking sodium reabsorption here, they accidentally cause lithium to be reabsorbed too. This can increase lithium levels by 25% to 40%. Loop diuretics like furosemide act higher up in the kidney, so they interfere less with lithium reabsorption. While furosemide still raises lithium levels (by 10% to 25%), it’s generally considered safer than thiazides for patients on lithium.
How often should lithium levels be checked when starting a new drug?
When you start a new medication that interacts with lithium - like a diuretic or NSAID - your lithium level should be checked every 4 to 5 days for the first week. After that, weekly checks for the first month are recommended. Once levels stabilize, you can return to routine monitoring every 3 to 6 months. Never assume your level is still safe just because you’ve been on lithium for years. New drugs change everything.
What are the early signs of lithium toxicity?
Early signs include hand tremors, increased thirst, frequent urination, mild nausea, and fatigue. These can be mistaken for side effects of bipolar disorder or aging. As toxicity worsens, symptoms become more serious: muscle weakness, slurred speech, confusion, dizziness, blurred vision, or seizures. If you notice any of these, get your lithium level checked immediately. Don’t wait for symptoms to get worse.
Can lithium toxicity be reversed?
Yes, but it depends on how severe it is. Mild toxicity (levels 1.5-2.0 mmol/L) often resolves by stopping the interacting drug and drinking more fluids. Moderate to severe toxicity (above 2.0 mmol/L) requires medical intervention - including IV fluids, stopping lithium, and sometimes hemodialysis. Even after blood levels drop, lithium can still be trapped in brain and nerve cells, so close monitoring for days after treatment is essential. Delayed relapse into toxicity is common.
Final Warning: Don’t Assume It’s Safe
Lithium isn’t going away. It’s still the only mood stabilizer proven to cut suicide risk by 44%. That’s why millions still take it. But that benefit comes with a price: constant vigilance. The drugs you take for your blood pressure, your arthritis, or your headache aren’t harmless when lithium is in your system. They’re landmines. You need to know which ones to avoid. You need to get tested. You need to speak up. Because if you don’t, the next time you feel a little off - it might not be just a bad day. It might be your body screaming that your lithium level just crossed the line into danger.


Milad Jawabra
March 5, 2026 AT 22:26Lithium is a beast. I’ve seen people go from chill to hospitalized in under a week because they popped Advil for a headache. No joke. Your body doesn’t care if it’s ‘just’ OTC - lithium doesn’t negotiate. If you’re on it, treat every new pill like a grenade. And yeah, I’m yelling at you, too. Stop assuming. Start testing. 🚨
Raman Kapri
March 6, 2026 AT 06:38While the clinical data presented is statistically significant, one must question the generalizability of these case studies. The sample sizes referenced are anecdotal, and the extrapolation to broad populations lacks longitudinal validation. Furthermore, the assertion that NSAIDs uniformly elevate lithium levels ignores pharmacogenetic variability in renal transporters. A more nuanced approach is warranted.
Tildi Fletes
March 6, 2026 AT 20:50Thank you for this meticulously referenced piece. The distinction between thiazide and loop diuretics is critical, and I appreciate the emphasis on eGFR monitoring. For clinicians, this is a textbook example of polypharmacy risk. I would add that patients with CKD Stage 3+ should avoid thiazides entirely when on lithium - even if BP control is challenging. Documentation of shared decision-making is non-negotiable.
Sharon Lammas
March 7, 2026 AT 11:24It’s haunting how something meant to stabilize your mind can quietly unravel your body. I’ve sat with people who didn’t know their lithium level had been creeping up for months because they ‘felt fine.’ The tragedy isn’t the toxicity - it’s the silence around it. We treat mental health like a checkbox, not a living system. Maybe if we talked about the body as part of the mind, fewer people would slip through.
Aisling Maguire
March 9, 2026 AT 09:49Bro. I took ibuprofen for my period last month and didn’t think twice. Then I got dizzy, nauseous, and my hands wouldn’t stop shaking. Thought I was dying. Went to the ER - lithium was at 2.1. They had to pump my stomach. I’m lucky I didn’t get brain damage. If you’re on lithium and you think you’re immune to this? You’re not. Stop being a hero. Get tested.
Diane Croft
March 10, 2026 AT 10:50You’re not alone. I’ve been on lithium for 12 years. I check my levels religiously. I use Tylenol. I tell every new doctor - even the dermatologist. It’s not paranoia. It’s survival. And if you’re scared to speak up? You’re not weak. You’re just not informed. Let’s change that.
tatiana verdesoto
March 12, 2026 AT 09:23I’m a nurse who works with psychiatric patients. I’ve seen this happen too many times. Someone’s on lithium, gets a UTI, gets prescribed Bactrim - which also messes with kidney clearance. They get confused, fall, fracture their hip. It’s not ‘just’ a side effect. It’s a cascade. We need better alerts in EHRs. And we need to stop blaming patients for not knowing. They’re not doctors.
Siri Elena
March 13, 2026 AT 07:12Oh honey. You mean to tell me that a drug that’s been around since the 1940s has *side effects*? Shocking. Next you’ll tell me oxygen can kill you if you’re on a ventilator. At least this post had a bibliography. I’m impressed. *claps slowly* Now go get your lithium level checked, sweetie.
Renee Jackson
March 13, 2026 AT 20:56As a clinical pharmacist with over two decades of experience in psychopharmacology, I must emphasize that the interaction between lithium and NSAIDs is not merely pharmacokinetic - it is pharmacodynamic as well. The reduction in renal perfusion alters not only excretion, but also the distribution of lithium in the central nervous system. This necessitates not only monitoring, but also patient education protocols standardized across healthcare systems.
RacRac Rachel
March 15, 2026 AT 17:03Just wanted to say - if you’re reading this and you’re on lithium… you’re doing better than you think. 💪 Seriously. This stuff is scary, but you’re not alone. I’ve been on it for 8 years. I got my levels checked before my last vacation. I use ginger tea for headaches. I tell my friends. And I’m still here. You’ve got this. One lab test at a time.
Richard Elric5111
March 16, 2026 AT 23:58One cannot help but contemplate the ontological paradox of lithium: a substance that stabilizes the mind by destabilizing the body. Is this not the essence of modern psychiatry? We intervene with chemicals that demand constant surveillance, while society insists on convenience. The body, after all, is not a machine to be optimized - it is a temple of biochemistry, and lithium is a priest who demands daily sacrifice. The irony? The very drug that grants lucidity may require the surrender of autonomy.
Dean Jones
March 18, 2026 AT 04:41I’ve been on lithium since I was 21. Now I’m 53. I’ve had two near misses. Once when I took naproxen for a back sprain - didn’t tell my psych. I woke up at 3 a.m. thinking my tongue was melting. Went to the ER. Level was 2.4. They gave me fluids and kept me overnight. Another time, my doc switched me from furosemide to hydrochlorothiazide for edema. Said it was ‘better for blood pressure.’ Didn’t even check my level for 10 days. I almost died. I’m not exaggerating. I had slurred speech for three days. My hands shook like I had Parkinson’s. My wife said I looked like I was drunk. I wasn’t. I was poisoned. And no one warned me. Not the pharmacist. Not the primary. Not the nurse. Just a Reddit post I found two years later. I’m still mad. If you’re on lithium - don’t wait for a post. Talk to someone. Now.
Betsy Silverman
March 19, 2026 AT 16:12I’m from a small town in the Midwest. We don’t have psych clinics. My psychiatrist is 90 minutes away. I do my own blood draws now - I have a kit. I send the results in. My doc reviews them. It’s not perfect, but it’s better than nothing. If you live somewhere rural, don’t give up. There are ways. Ask your pharmacist. Call your psych. Text someone. You’re worth the effort.
Ivan Viktor
March 20, 2026 AT 06:33So… you’re telling me I can’t take my daily ibuprofen for my knee? What am I supposed to do, sit around in pain? And who even reads these long-ass posts? I’m just here for the memes. 🤷♂️